Health equity
Rhian Last, RN
Rhian Last, RN
Associate, Experience Led Care Programme, RCGP Yorkshire Faculty Board Member, Self Care Forum Board Member
The health gap between deprived and well off parts of the country has widened, and once we get through this pandemic, can only be expected to become worse. Here we look at health inequality, explore the social determinants of health and the practical measures that GPNs can implement to make a positive impact on health equity in their local community
A decade ago, a review entitled Fair Society, Healthy Lives set out six priorities for improving health:1
- Making sure that every child has the best start in life
- Enabling and empowering children, young people and adults to realise their full potential and have control of their lives
- Creating fair employment and meaningful work for all
- Making certain that everyone has a healthy standard of living
- Facilitating the development of healthy and sustainable places and communities
- Enhancing the prevention of ill health.
A follow up report, Health Equity in England, The Marmot Review 10 Years On was published this year, with some salutary findings.
People can expect to spend more of their lives in poor health, improvements in life expectancy have stalled, and have worsened for the poorest 10% of women. The health gap between deprived and wealthier areas of the country has actually widened. In essence, it has been established that, far from making progress towards more equality, things have deteriorated in many areas. The impact of deprivation on a person’s health is worse for a person living in a deprived area of the North East than for a person living in a comparably deprived area of London, to the extent that life expectancy can differ by nearly five years.
The overall findings regarding outcomes and actions in England since 2010 are disappointing, but there are some causes for optimism. Since 2010 there has been a significant increase in awareness of health inequalities and the social determinants of health, with some – albeit spasmodic – evidence of good practice.
SOCIAL DETERMINANTS OF HEALTH
These are the conditions under which people are born, grow, live, work and age. These circumstances are moulded by the distribution of money, power and resources at global, national and local levels. There is much discussion about what can impact on these social determinants, and a challenging suggestion that it is not the inequalities that kill people but rather that it is those who are responsible for the inequalities.3 This responsibility may not always be at a high political level either. Are there, for example, any decisions made in your own practice that could impact unequally on the disadvantaged, such as access to information for those with poor literacy or inability to access information online?
The latest report identified key causes for current concern:2
- Child poverty
- The housing crisis
- The rise in homelessness
- People with insufficient money to lead a healthy life.
Food insecurity
Food insecurity is the state of being unable to access a regular, reliable source of affordable nutrition due to lack of money. Put simply, it means never quite knowing where your next meal will come from.
The State of Hunger Report in 2019,4 found the prevalence of food insecurity among children was higher than among adults: around 11% of children lived in food insecure households, and women living in a couple with children also tended to be more food insecure than the men, because they were more likely to miss meals so their children have enough to eat.
The chance of being food insecure was higher among:
- Households with lower incomes
- The unemployed
- Younger people
- Lone-parent households or single-person households
- Households who rented (particularly those in social housing)
- People affected by ill health.
A significant 94% of those using food banks also met the definition of being destitute.5
The housing crisis
The latest Marmot report,2 found poor quality housing, particularly cold, damp homes, can cause direct harm to both physical and mental health. Poor housing conditions continue to contribute to health harm and a widening of health inequality.
Unaffordable housing also has a detrimental effect on health. Around 21% of adults in England reported that a housing issue had had a negative impact on their mental health, even where they reported no previous mental health issues. Housing affordability was frequently the reason given. Rising stress levels as a result of falling behind with housing payments are on a par with those from unemployment.
Housing costs in England have increased significantly since 2010 and the impact is greater on lower income families. The cost of social renting in in England increased by 40% between 2008 and 2016 and a third of households in the private rental sector fall into poverty because of their housing expense.
The anxiety around trying to meet housing costs will have resulted in worsening health for low income families.
Prescription costs
With an ever increasing prevalence of long term conditions some people can find themselves on multiple, long term medications. Some people are entitled to free prescriptions, and there are also various ways that people can get help with arranging their prescription payments. As general practice nurses (GPNs) it’s important that we don’t assume that people will understand the options that might be available to them to assist with this. Even in seemingly well-off areas, individuals can have money problems, so information about these options should be readily available in every GP practice. (See Resources)
When patients do find they are financially compromised they can often take risks by rationing their medicines or even leaving some out altogether. This is not information that they will necessarily wish to share with healthcare professionals (HCPs). You can listen to a recent, insightful patient story about prescription costs here.
Perhaps the biggest inequality of all with regard to prescription charges is that in Scotland, Wales and Northern Ireland all prescriptions are dispensed free of charge to the patient. This places people living in England at a disadvantage.
MARGINALISED COMMUNITIES
Marginalised communities will include:
- The homeless
- Sex workers
- Lesbian, gay, bisexual and transgender (LGBT) people
- Refugees and asylum seekers
- Gypsy and traveller groups.
Applying an outreach model of care delivery, where HCPs go out to the people and their community groups rather than calling people in to a designated centre, can have a positive impact on care delivery and improving health outcomes.6
The homeless
Homeless people need a holistic approach to their care, and effective coordination of care that acknowledges and addresses chaotic lives.
The Queens’ Nursing Institute has developed a template for assessing the health of people who are homeless, which covers general physical health, long term conditions, substance use, mental health, sexual health and housing. It incorporates plans for use by both nurses and patients. The guidance was informed by people who have lived experience of homelessness and was created by community nurses specialising in homeless health. It meets national guidelines including existing NICE standards, Public Health England outcomes on homeless health, and the standards for commissioners and service providers by the Faculty for Homeless and Inclusion in Health. You can access the template here.
Some nurses work in practices that are specifically designated centres for homeless people. However, homelessness can impact on patients in any GP surgery and is not confined to people living on the streets or in shelters for the homeless. There are people – the so-called ‘sofa surfers’ – who live on a variety of friends’ couches, without having a firm home base.
People can lose their home at any and all ages, and in many different social circumstances. They will often try to hide the situation from family and friends and may well continue to attend their existing general practice surgery for repeat prescriptions while living on the streets many miles away.7 There will be an associated fear of being judged.8
A wish to hide their homelessness or a fear of being judged are very important reasons for us to change our consultation style so that we can pick up cues from someone who might be living in distressed circumstances. This will be explored later in more detail.
Learning disability
We also need to give full consideration to people who are living with learning disability. They have poorer physical and mental health and die younger than other people.
In primary care everyone with learning disability is entitled to an annual health check. This needs to be a positive and meaningful experience for the patient concerned and for their family members or carers, who may also be involved. In some circumstances it may be more appropriate for the patient if the review is undertaken in the environment most comfortable for them, for example as a home visit perhaps. The Royal College of General Practitioners (RCGP) has produced a toolkit to support best practice in health checks for people with learning disability. (See Resources)
Period poverty: some positive news
Findings from research undertaken by Plan International UK in 2017 indicated the following:9
- 10% of girls have been unable to afford sanitary wear
- 15% have struggled to afford sanitary wear
- 14% have had to ask to borrow sanitary wear from a friend due to affordability issues
- 12% have had to improvise sanitary wear due to affordability issues
- 19% of girls have changed to a less suitable sanitary product due to cost.
In the recent Budget (March 2020) the Government announced that free sanitary products would be available in schools in England from 2020,10 and VAT on sanitary products would be removed at the end of this year.11
Another group of people who can find themselves compromised by lack of access to appropriate sanitary wear are hospital patients. In March 2019 it was announced that NHS England is to offer free tampons and other sanitary products to any patient who needs them. This will go some way to ensuring dignity and peace of mind at a vulnerable time. You can find out more here.
YOUR ROLE IN SUPPORTING HEALTH EQUITY
Narrative competence
We can gain far greater insights into life in general for our patients by adopting a holistic approach, through taking a social history in addition to a clinical history. Each patient has their own unique story, which includes their conditions, their new problem, their social situation, and their beliefs.12
It is also extremely important to gain an understanding of our patients’ perspectives of their health and wellbeing by actively listening to their narrative.13 We are more likely to elicit conversation if we use open, rather than closed questions which tend to prompt only yes or no responses. This method of drawing out a patient’s story has been described as narrative competence. This engenders empathy, reflection, professionalism, and trustworthiness in a health professional.14 These are important strengths to enable meaningful engagement.
We need to facilitate good, effective and relevant, personalised care by ensuring that everyone is given the opportunity to be involved in decisions about them and their health and social care.15 The attitude and approach to patient care, where we view ‘them’ consulting ‘us’, might be improved if we view this from a different stance: ‘We are not hosts in our organisations so much as we are guests in our patients’ lives.’16
Health Literacy
Health literacy can be defined as the degree to which a person has the capacity to obtain, assimilate and understand health information and services to support them in making appropriate decisions about their health. This is a complex concept which ranges from basic skills in reading and numeracy through to the cognitive skills needed to process information and apply this to facilitate personal control over events and situations. Appreciating the compromises faced by people with low health literacy can help to reduce inequalities.17 Sourcing information that is easy to read and understand will be helpful for patients and will support informed consent.
However, it is not simply the giving of the information that is important, but it is knowing that the patient has understood the information they have been given.18 We can do this by checking back, asking the patient to reflect back in their own words what has been shared and discussed. That way any misunderstandings or misconceptions can be clarified and corrected.
Asset based approaches in consultation
Very often we open our consultations with ‘How can I help you today?’ or ‘What is the problem?’. This sets a stance of ‘needs’ and prompts people to think about what is lacking in their life. This can promote a downward spiral of thinking where they can lose sight of what is good in their life, their ‘assets’ or ‘strengths’.
If you open a conversation by asking ‘What is going well, right now?’ that is to say, the ‘strengths’ that are working in someone’s favour, then the stance is reversed to become more positive, thereby promoting a wellbeing conversation.19
Social prescribing
Social prescribing enables healthcare professionals to address non-medical causes of ill health through signposting and utilising the resources of the voluntary and community sectors.20
Social prescribing is becoming widely promoted in the UK as a way of addressing complex health, psychological and social issues that present in primary care, improving support for people with long term conditions and facilitating sustainability in general practice. Importantly, it is also regarded as an intervention with the potential to reduce health inequalities.21
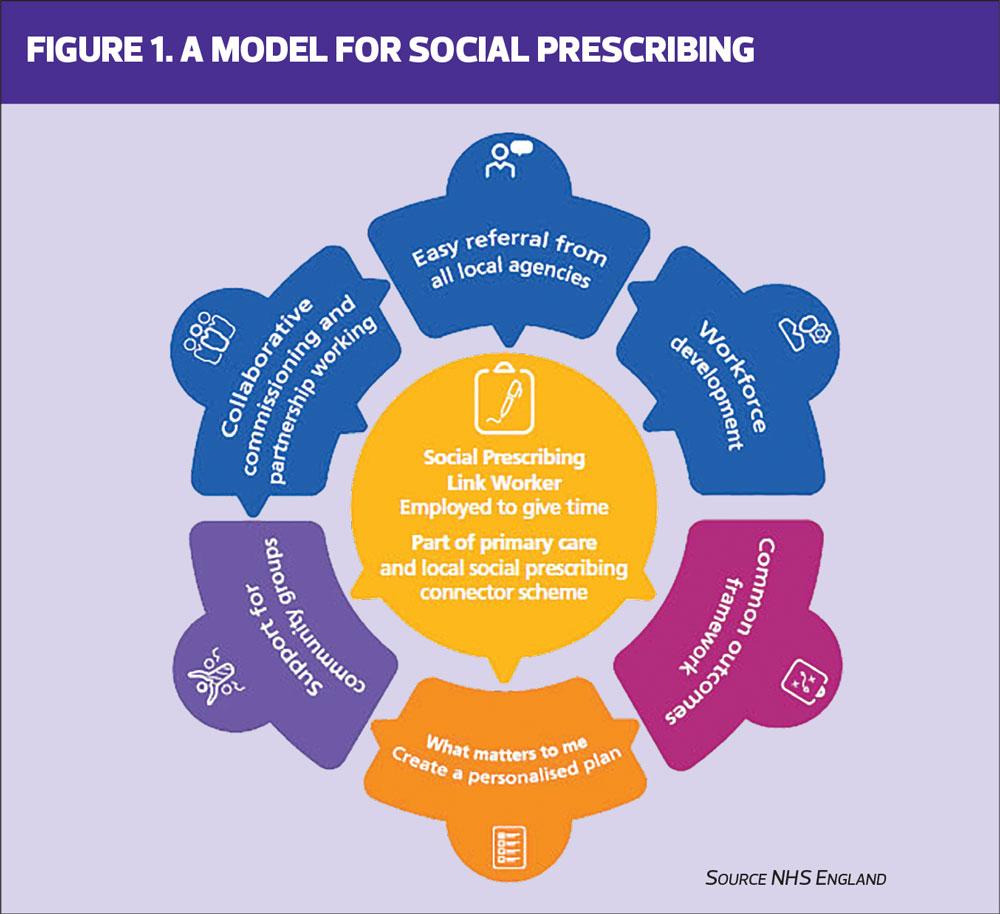
A standard model of social prescribing has been developed by NHS England in partnership with stakeholders, which demonstrates the key elements that need to be in place to facilitate effective social prescribing. (Figure 1)
Frequent attenders
Frequent attenders in general practice can benefit from more intense, meaningful conversations which gather a better overall insight into their life story and a greater understanding as to why they are presenting regularly at the surgery.22 These individuals very often have unmet needs which require further consideration. Social isolation has been associated with frequent attendance and interventions that promote social group connection have shown promise for reducing overuse of GP services.23 Social prescribing can play a big part here.
Group consultations
Another interesting, new approach to patient care are group consultations for long term conditions. These offer patients the opportunity to discuss and review their condition in a group setting rather than in the traditional one-to-one consultation. There is an emerging evidence base of improved outcomes, better patient experience and more effective time management with this approach.24 (See Further Reading and Resources for links to patient stories and case studies)
Collaborative Working
In January 2019, a five year GP contract framework was agreed, with the intention of stabilising general practice and facilitating delivery of the NHS Long Term Plan.25,26 There was an extension to the contract, in the form of a direct enhanced service (DES) and this would be offered to general practices to enable them to form primary care networks (PCNs), generally covering populations of around 30,000 to 50,000 people. Among the seven national service specifications were to be initiatives to tackle inequalities (to be agreed at local level). This had been expected to involve collaborative working across health and social care together, understanding the demographics of the local population and useful application of data and analytics to understand what is good and what might be improved regarding health equity in the PCN locality. However, this – together with CVD diagnosis and prevention, personalised care and anticipatory care – has now been deferred to 2021-22, following renegotiation with the BMA’s GP committee.27
SUMMARY
The recent Marmot report, Health Equity in England, the Marmot review 10 years on, made for uncomfortable reading and articulated an urgent imperative for us all to take action and do better at reducing inequalities in health. This article has examined the key areas of concern highlighted in the report and explored them from the perspectives of national policy, PCNs and, importantly, from the perspective of the GPN in front line general practice.
We all need to take action to ensure that, 10 years from now, we will be living in a more humane and equal society that holds health equity at its very core.
REFERENCES
1. Marmot M, Allen J, Goldblatt P, et al. Fair Society, Healthy Lives: The Marmot Review. London; 2010.
2. Institute of Health Equity. Health Equity in England, the Marmot review 10 years on. 2020. http://www.instituteofhealthequity.org/resources-reports/marmot-review-10-years-on/the-marmot-review-10-years-on-full-report.pdf
3. Navarro V. (2009). What We Mean by Social Determinants of Health. Int J Health Serv. 2009;39(3):423-441.
4. The Trussell Trust. The State of Hunger; 2020 https://www.trusselltrust.org/wp-content/uploads/sites/2/2019/06/SoH-Interim-Report-Final-2.pdf
5. Fitzpatrick S, Bramley G, Sosenko F, et al. Destitution in the UK 2018. Joseph Rowntree Foundation. York; 2018 https://www.jrf.org.uk/report/destitution-uk-2018
6. Keat L. Improving access to health care for gypsy and traveller communities. GPN Journal. 2018;4(4):63-5 https://www.journalofpracticenursing.co.uk/files/downloads/articles/15---improving-access-to-health-care-for-gypsy-and-traveller-communities.pdf
7. Courtenay T. Four Feet Under: Thirty untold stories of homelessness in London Unbound. 2018. ISBN: 9781783525720
8. Wilkinson R, Pickett K. The Spirit Level: Why Equality is Better for Everyone. Penguin. London. 2009
9. Plan International UK. Plan International UK's research on period poverty and stigma. 2020. https://plan-uk.org/media-centre/plan-international-uks-research-on-period-poverty-and-stigma
10. Adams R. Free period products to be available in schools in England. The Guardian. 18th Jan 2020. https://www.theguardian.com/education/2020/jan/18/free-period-products-to-be-available-in-schools-and-colleges-in-england
11. Gov.UK. Budget 2020. What you need to know. https://www.gov.uk/government/news/budget-2020-what-you-need-to-know
12. Centor RM. To be a great physician, you must understand the whole story. MedGenMed. 2007;9(1):59
13. Greenhalgh T, Hurwitz B. Narrative-Based Medicine. BMJ Books, London. 2004
14. Charon R. The narrative road to empathy. In: Spiro H, Curnen MGM, Peschel E, et al, eds. Empathy and the Practice of Medicine: Beyond Pills and the Scalpel. NewHaven, Yale University Press 1993. 147–59
15. Last, R. Making personalised care happen: implementing the 'Comprehensive Model' in general practice. Practice Nurse 2019;49(9):33-37
16. Berwick DM. (2002) Escape Fire: Lessons for the Future of Healthcare. The commonwealth Fund 2002. https://www.commonwealthfund.org/sites/default/files/documents/___media_files_publications_other_2002_nov_escape_fire__lessons_for_the_future_of_health_care_berwick_escapefire_563_pdf.pdf
17. Rowlands G. Health literacy. Hum Vaccin Immunother. 2014;10(7):2130–2135. doi:10.4161/hv.29603
18. Elwyn G, Edwards A, Wensing M, et al. Shared decision making: developing the OPTION scale for measuring patient involvement. Qual Saf Health Care. 2003;12(2): 93–9
19. Henry H,Howarth ML. An overview of using an asset-based approach to nursing. General Practice Nursing. 2018;4(4):61-66.
20. Polley M, Berttotti M, Kimberlee R,et al. A review of the evidence assessing impact of social prescribing on healthcare demand and cost implications. London: University of Westminster. 2017. https://westminsterresearch.westminster.ac.uk/download/e18716e6c96cc93153baa8e757f8feb602fe99539fa281433535f89af85fb550/297582/review-of-evidence-assessing-impact-of-social-prescribing.pdf
21. South J, Higgins TJ, Woodall J, et al. Can social prescribing provide the missing link? Prim Health Care Res Dev 2008;9:310–18 doi:10.1017/S146342360800087X
22. Nettleton S. ‘I just want permission to be ill’: Towards a sociology of medically unexplained symptoms. Social Sci Med. 2006;62:1167-78.
23. Cruwys T, Wakefield J, Sani F, et al. Social Isolation Predicts Frequent Attendance in Primary Care. Ann Behav Med. 2018;52(10):817-829.
24. Bostock B, Brady L, Hodgson EK. Group consultations: the why and the how. Practice Nurse 2019;49(4):34-7
25. NHS England. A five-year framework for GP contract reform to implement The NHS Long Term Plan; January 2019. https://www.england.nhs.uk/publication/gp-contract-five-year-framework/
26. NHS England. NHS Long Term Plan; 2020 https://www.longtermplan.nhs.uk/
27. NHS England. Update to the GP contract agreement 2020/21 – 2023/24; February 2020. https://www.england.nhs.uk/wp-content/uploads/2020/03/update-to-the-gp-contract-agreement-v2-updated.pdf
Related articles
View all Articles