RESPIRATORY DISORDERSThe respiratory tract is considered in two parts, upper and lower. The upper respiratory tract (URT) comprises:
The lower respiratory tract (LRT) comprises:
Role of the respiratory systemThe prime function of the respiratory system is to maintain the exchange of oxygen and carbon dioxide in the lungs and tissues, and regulate the acid-base balance. Any change in this system will affect, and may present in, other body systems. Gas exchange between air and the bloodstream is a rapid process that takes place in the alveoli. An adequate supply of oxygen to the tissues depends on sufficient ventilation (air flow) and perfusion (blood flow) of the lungs. Impairment of either, e.g. by airway narrowing in uncontrolled asthma or left ventricular failure, may reduce the oxygen supply and lead to a raised concentration of carbon dioxide in the blood. Respiratory disordersMore than 40 conditions affect the lungs and/or airways, and respiratory disease causes one in five deaths in the UK. In addition:
Practice Nurse Curriculum Modules - Respiratory Disease
Diagnostic criteria in asthma & COPD Optimising therapy in asthma & COPD Respiratory disease: Signs and symptoms Respiratory diseases: Guidelines and Management
Asthma+Lung UK. Lung conditions Information for patients. https://www.blf.org.uk/support-for-you Health and Safety Executive. Prevent work-related lung disease https://www.hse.gov.uk/lung-disease/index.htm Primary Care Respiratory Society UK (PCRS-UK) https://www.pcrs-uk.org British Thoracic Society https://www.brit-thoracic.org.uk/ INTERSTITIAL LUNG DISEASEVariety of conditions causing gradually progressive shortness of breath and cough. Many different causes, but a common feature is deposition throughout the lungs of fibrous material that destroys lung tissue. Examples are: Dust-related diseases, e.g. Coal worker's pneumoconiosis, asbestosis Extrinsic allergic alveolitis (hypersensitivity pneumonitis), eg pigeon fancier’s lung, farmer’s lung Idiopathic pulmonary fibrosis (cryptogenic fibrosing alveolitis) Primary disease, e.g. sarcoidosis
NICE CG163 Idiopathic pulmonary fibrosis in adults: diagnosis and management; 2013 (updated 2017) https://www.nice.org.uk/Guidance/CG163 Practice Nurse featured article
Interstitial Lung Disease Jane Scullion
LUNG CANCERDisease in which there is progressive multiplication of cells (neoplasia) under conditions where this would not normally occur. When a malignant tumour forms, its cells are invasive, lose their differentiation and orientation, and disperse to parts of the body distant from the initial growth (metastasise). Cancer’s natural course is fatal. In most cancers, early detection and treatment increases the chance of survival. Lung cancer is the second most common cancer in the UK, and by far the biggest cause is smoking, causing 8 out of 10 cases. The 2 main groups of primary lung cancer are: Small cell lung cancer – so called because under the microscope the cells appear small and mostly taken up by the nucleus. Accounts for 12% of lung cancers and very rare in people who have never smoked. Non small cell lung cancer – includes squamous cell carcinoma, adenocarcinoma and large cell carcinoma. Secondary lung cancer is frequently associated with breast or bowel cancer that has metastasised. Treatment depends on the where the cancer originated. Cancer Research UK. About cancer https://www.cancerresearchuk.org/about-cancer Macmillan Cancer Support. Cancer A to Z https://www.macmillan.org.uk/cancer-information-and-support NICE NG12. Suspected cancer: recognition and referral; 2015 (updated 2021) https://www.nice.org.uk/guidance/ng12 Cancer treatments include surgery, radiotherapy and chemotherapy. Adverse effects of therapy include immunosuppression, and hence susceptibility to infection, and more specific problems such as sore mouth and eating problems with radiotherapy to the head and neck, and hair loss with chemotherapy. Patients will see specialist staff but may appreciate additional support and help with accessing resources. RESPIRATORY TRACT INFECTIONS (RTIs)Most common RTIs are self-limiting viral infections that clear up fairly quickly in previously well patients, needing only simple self-help advice or OTC remedies. Patients will not benefit from an antibiotic unless their symptoms are caused by bacterial rather than viral infection (clinical distinction is often not possible), or they are at risk of complications from the infection. URTIs cause considerable discomfort but rarely death or serious illness. LRTIs are usually more serious, and particularly common and serious in the elderly. Certain infections, such as influenza, can affect both the upper and lower respiratory tract. NICE NG120. Cough (acute): antimicrobial prescribing; 2019 https://www.nice.org.uk/guidance/ng120 Acute bronchitisInflammation of the bronchial tree. Common in winter; generally a complication of viral upper respiratory infection (common cold, sore throat or influenza). Presents with hacking cough, usually bringing up yellowy-grey mucus; may be pyrexia, retrosternal pain and wheeze, rhonchi, coarse crepitations.
Practice Nurse featured article Cough: not always what it seems Margaret Perry Common cold
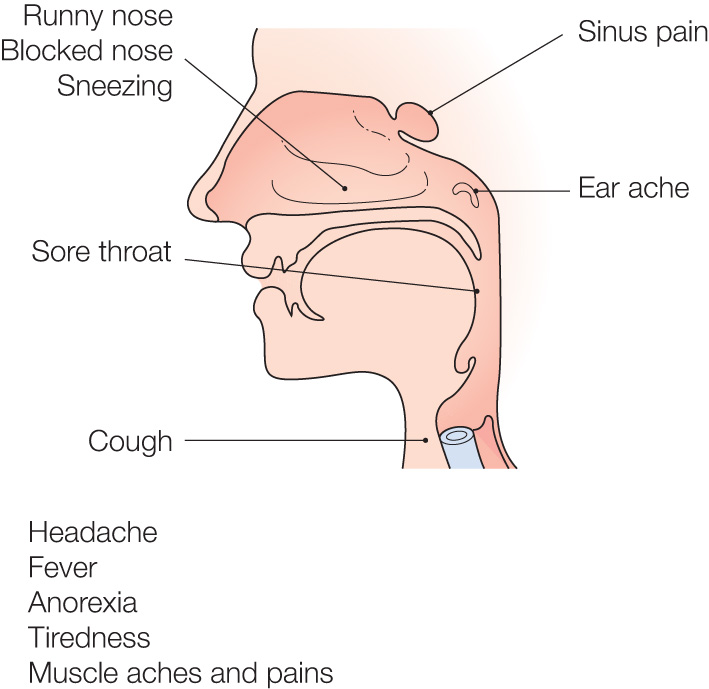
A viral infection of the nose and throat, and the most common acute illness in the industrialised world. Adults generally have 2-4 colds per year, children up to 12. Young children are main reservoir of the causative viruses. Symptoms of the common cold syndrome are caused by >200 different viruses. Rhinoviruses (nose viruses) account for c. 30-50% of adult colds; others include coronavirus, respiratory syncytial virus (RSV), adenovirus, parainfluenza virus, influenza virus.
Practice Nurse featured article Nasal congestion Dr Knut Schroeder, Sara Richards Croup (laryngotracheitis)Infection of the larynx and trachea, with laryngeal oedema and obstruction of airway by thick, tenacious secretions. Presents with barking cough of sudden onset, usually inspiratory stridor, often hoarseness, respiratory distress. Usually affects children between 6 months and 3 years old InfluenzaHighly contagious acute viral infection of the upper respiratory tract. Onset is sudden, symptoms include headache, myalgia, fever and cough. Spread is by droplet, person-to-person contact or contact with contaminated items, e.g. door handles. May predispose to secondary bacterial infection of the upper and lower respiratory tract. Most recover in 1–2 weeks without complications but ‘flu’ can cause serious illness and death, especially in very young, elderly or infirm. Influenza occurs most often in winter and usually peaks December–March in the northern hemisphere. Every 2–3 years epidemics occur, and mortality may be high. Practice Nurse featured article How viruses attack: the story and history of influenza Beverley Bostock-Cox Top tips for patients to help combat flu Sara Richards LaryngitisInflammation of the larynx. Presents with hoarseness, loss of voice, sore throat.
Refer urgently patients with hoarseness persisting >3 weeks PneumoniaInflammatory infection of the bronchioles and alveoli. Community-acquired pneumonia (CAP) occurs in 1 in 100 of the population each year, twice as common in winter, highest rates in elderly and young. About 10% is viral; most common bacterial causes are: Streptococcus pneumoniae (pneumococcus), Mycoplasma pneumoniae, Haemophilus influenzae. Infections with Legionella pneumophila are generally the result of droplet infection from an air-conditioning system. NICE NG138. Pneumonia (community-acquired): antimicrobial prescribing; 2019 https://www.nice.org.uk/guidance/ng138 Hospital-acquired pneumonia develops in up to 50% of patients, mortality rate is high. Organisms commonly identified are pneumococcus, Staphylococcus aureus, and Gram-negative bacteria (Pseudomonas, Klebsiella, Proteus). SinusitisInflamed or infected sinuses. Often follows an acute viral URTI. Inflammation of mucous membranes of paranasal sinuses can result from inadequate drainage of sinuses secondary to infection, allergy or obstruction. May present with headache, pyrexia, localised pain (worse when bending forward) and tenderness over involved sinus. Complications, e.g. facial or periorbital cellulitis, are more common in children than in adults. Sore throat/tonsillitisIncidence peaks at 5-10 and 15-25 years. Spectrum includes laryngitis, pharyngitis and, in a few, tonsillitis; clinical distinction between the last two not always clear. Streptococcal tonsillitis more likely if patient is less than 11 years old, with myalgia, fever history, tonsillar exudates, tender or swollen cervical lymph glands, less likely if cough/earache present. If recurrent sore throat very troublesome, e.g. child often misses school, tonsillectomy may be indicated but is not undertaken lightly. ENT UK. Commissioning guide: Tonsillectomy; 2021 Snoring and obstructive sleep apnoeaSnoring is the vibratory noise generated from the pharynx and soft palate during sleep. Apnoea is a temporary absence or cessation of breathing. Obstructive sleep apnoea (OSA) occurs when complete closure of the pharyngeal airway causes repeated episodes of apnoea and transient arousal. The result is fragmented sleep and excessive daytime sleepiness, making it dangerous for those affected to drive or operate machinery. Causes include overweight (neck circumference >16in), nasal congestion, evening alcohol/sedatives, large tonsils, receding lower jaw. Patients diagnosed with OSA should be referred to a sleep unit or physician with a special interest in sleep problems. OSA may be improved by lifestyle changes such as weight loss, smoking cessation, changes in sleeping position and avoidance of alcohol or night sedation tablets. Continuous positive airway pressure (CPAP) is most commonly used for severe OSA. NICE TA139 Continuous positive airway pressure (CPAP) for treatment of obstructive sleep apnoea/hypopnoea syndrome, 2008 https://www.nice.org.uk/guidance/TA139 NICE Guideline in development. Obstructive sleep apnoea/hypopnoea syndrome and obesity hypoventilation syndrome. Expected publication date: August 2021. Draft for consultation, March 2021. https://www.nice.org.uk/guidance/gid-ng10098/documents/draft-guideline Practice Nurse featured article
Sleep apnoea: assessment and management. Dr Gerry Morrow
Certain signs and symptoms are indicative of more serious respiratory disease
|
|

 NICE NG12. Suspected cancer: recognition and referral; 2015 (updated 2021)
NICE NG12. Suspected cancer: recognition and referral; 2015 (updated 2021)